Surviving My First Week in Telehealth AAC Intervention!
Let’s be honest! Who isn’t freaking out just a little about doing AAC therapy via Telehealth? This #stayhome scenario is challenging! We are all under tremendous levels of stress at the moment; worrying about the world and finding a new routine for ourselves and our families.
Parents are struggling with home schooling and establishing new routines, many of our clients are confused and anxious about what is going on and why they cannot see their friends and as speech pathologists, we also having to re-invent our service delivery model and come up with new and engaging ways to do what we do best! I have found the last few weeks to be some of the most challenging of my career, but I must say it has also been fun and rewarding. So I thought I would share with you my learnings from the last few weeks as an AAC speechie. Hopefully you can take away some tips and ideas becuase #yougotthis!
Your families are likely to be asking the same questions as you
What preparation do I need to do before the video session? What tools do I need? How long should the session be?
What activities will work best by telehealth? What do I show on the screen? Me? Their device? The activity?
How do I adjust what I usually do to suit this new way of engaging in therapy?
Will my client be suitable for telehealth? Will they even look at the screen? Who will support the client at their end?
As the therapist, I felt like I needed to have all the answers to be able to best support my families. This is a lot of pressure! But it turns out, once I started talking to my families about Telehealth, they had exactly the same questions. There is no one size fits all! The best advice I can give you is to make the time to answer these questions together. A ten-minute phone call before your first session can put everyone’s mind at ease. Many of my families appreciated the time to talk through what a telehealth session might look like for them. We talked about who would be needed on their end of the call, what their roles would be, what resources were available at home and how long we might expect that we could engage their child for. We agreed on the most suitable time for the session, perhaps when the support worker was there or late morning once other siblings were settled into their home schooling for the day. For some families, we agreed that we would start with parent coaching sessions. For others, I agreed to send some activities by post or email before the session so the parent/carer could feel more prepared. The fact is, that we made these decisions about our telehealth journey together, and everyone felt more comfortable moving forward. Technology wise, I ensured that families felt supported and we did some test calls to check everyone was comfortable and we could hear and see each other. Even deciding where to position the camera was critical for some clients and we didn’t always get it right the first time. In the end, some sessions went great and others not so much, but we did it together. We made adjustments. I proactively sought feedback from families at the end of each session - what worked well and what didn’t, and we agreed on how we do things differently next time. Sometimes we agreed on the activities for the next session so everyone could feel prepared.
Never say never- telehealth is more than sitting quietly in front of a screen!
When I was reviewing my caseload, I was concerned that some of my clients with complex needs might not be suitable for telehealth. Sitting still and listening to me through a screen just didn’t seem possible! One client’s mum said to me “let’s just give it a go!” So we did, and I was blown away with how her daughter engaged with me on the screen - more so than in face to face therapy! She was attentive, listened well and moved her attention from me to her device. It helped that she was well positioned in her custom seating and supported to engage in the activities by her Mum and support worker. We had previously agreed on the different roles that we would take on in the session. For example, her support worker would be helping her to access with her device, Mum would be modelling the target vocabulary and I would be the communication partner asking questions and directing the activity. We agreed on sensory breaks at different times which the support worker facilitated and I used this time to chat with Mum and provide some ideas for embedding the targeted vocabulary within other activities during their week.
One of the most fun therapy sessions I’ve had in a while happened with another client, who is not the type to sit still. I am currently remotely supporting him to do an eye gaze device trial and last Friday, with his device positioned on the floor stand, he chose his favourite songs via eye gaze. While I played my drum and clapped along to Queen and Pop Goes The Weasel, he was dancing around the room with his mum and having a great old time. Check out his moves!

Though it can be tricky to monitor and support an AAC trial remotely, we have been using all the tools in our toolbox, including collecting video footage of device use, data logging, heat mapping to show eye gaze access and re-evaluating our clear and measurable goals to track progress. I have also been logging in to his device remotely using Team Viewer to complete programming and technical troubleshooting.
Spend the first ten minutes of the telehealth session preparing together
At the start of each session, I have learnt the value of using the first few minutes to make sure everyone knows what is going to happen - myself included. I might outline the session plan, agree on the activity and breaks if needed, ensure we have the AAC device and telehealth set up in the best position, and that the required toys or activities are available. We move people around to find the best camera angles for us to see each other and the device; I make sure I can see enough to be able to observe and modify the session as required. Sometimes, I chat with siblings who pop in and try to involve them as best I can by giving them a job to do, teach them to model on their brother or sister’s device or ask them to join in games and activities where appropriate.
I also use this first ten minutes to “prime” everyone for the goals and vocabulary in the session. I have found it helps to ensure the communication partners know which words or phrases we are working on and where to locate this vocabulary on the device. Parents’ feedback has been that this is really useful, and they feel more confident in modelling these words during and after the session. I usually bring up their vocabulary on my PASS or Chat Editor software, so they can follow along with me or I make up a Smart Chart in advance and share this on my screen.
Sometimes all the preparation in the world isn’t what you need!
I was feeling really confident about one session last week with a client who I have known for a really long time, who loves to Facetime with others. I had prepared activities that I was confident she would love and I knew her support worker, younger sister and Mum would be at the other end of the call to support with modelling and structuring the activities. It was going to be great. But, I was WRONG!
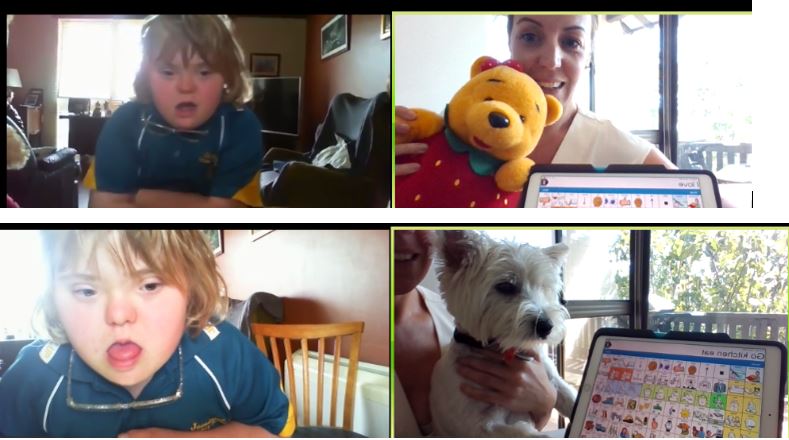
Despite my interactive iPad activities mirrored to the Zoom call, she was not interested at all and became upset and distracted within the first few minutes. She desperately wanted her sister to join in, who declined because she had her own school work to do. After about five minutes, her Mum suggested that she might like to see me, not my fancy iPad activity. Once I turned the camera to me and started to chat, she became a little more engaged. From here, I knew I had to think on my feet. I know she loves dogs so I asked if she wanted to meet my dog, Walter. She was immediately engaged and we got to work on her goal of learning to use more verbs. We practiced “kiss” when Walter was trying to lick me, “sleep” when the dog yawned and “go kitchen eat” when she thought Walter might like a treat.

After this, we started to chat about all the teddies that people are leaving in their windows. My client decided to get up and show me her toys, so I did the same. This gave us lots to talk about and her sister even joined in! The lesson learnt here was, sometimes you just have to go with the flow, scrap the fancy prepared activities and follow the client’s lead - just keep your goals in mind. You never know what exciting things there will be to talk about.

So in these uncertain times, here are my take away messages from week one in Telehealth AAC.
- Look after yourself – take breaks from the screen between meetings and look after your voice.
- Allow yourself the head space and ample planning time before a session to work through the logistics and session plan.
- Be clear on your goals and share these at the start of the session.
- Do a test of the technology and experiment with positioning yourself, the client/ family and screens/cameras so everyone gets the most out of it.
- Talk about the session plan, roles and responsibilities prior to your first session.
- You can be the best motivator for communication – put yourself on screen too, it’s not all fancy apps and virtual games.
- Go with the flow and follow the client’s lead.
If you are interested in more ideas about AAC intervention via Telehealth, you can check out my recent webinar https://www.youtube.com/watch?v=IGemQPamTkw&feature=emb_logo.
About Me… My name is Kelly Savage and I am a speechie who just loves AAC. I am currently working as an AAC Consultant and therapist for Liberator Australia and also have my own small private practice.
By Kelly Savage, AAC Consultant, Liberator Australia



